Understanding Unilateral Gynecomastia: Causes and Effective Treatment
When you notice that only one side of your chest appears larger or fuller than the other, you may be experiencing unilateral gynecomastia. This guide is for men and adolescent boys experiencing one-sided chest enlargement, as well as parents seeking information for their sons.
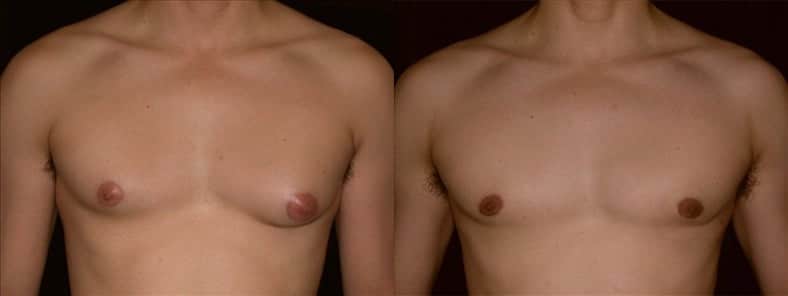
Addressing unilateral gynecomastia is important not only for physical health but also for emotional well-being and self-confidence. This condition—known as unilateral gynecomastia—affects more men than you might realize, yet it often goes unaddressed due to embarrassment or uncertainty about what to do. Understanding what causes one-sided breast enlargement and knowing that effective correction is available can be the first step toward regaining your confidence. In cases of unilateral gynecomastia, the affected male breast can closely resemble the female breast in appearance, which can increase emotional distress and is an important factor in both diagnosis and treatment planning.
Quick Overview: What Is One-Sided Gynecomastia?
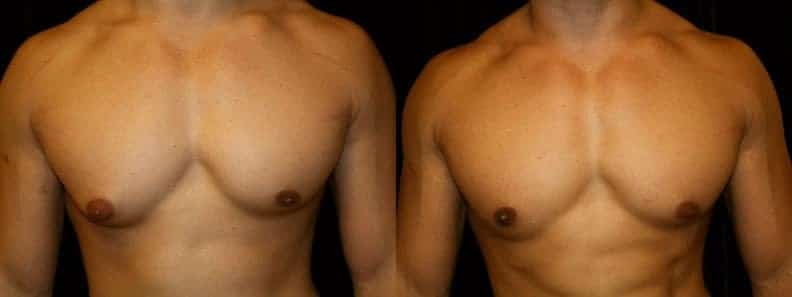
Unilateral gynecomastia refers to benign proliferation of glandular tissue in one breast in males, resulting in visible chest asymmetry. Unlike bilateral gynecomastia, where both sides are affected, this one-sided presentation means one half of your chest may look noticeably different from the other—sometimes dramatically so.
While most gynecomastia cases involve both breasts to some degree, studies suggest that roughly 10–35% of gynecomastia cases present unilaterally or with significant asymmetry. The condition itself is usually benign, but the emotional distress it causes can be profound. The breast ducts, which are present in male breast tissue, can also be involved in the development of symptoms or in the evaluation of underlying breast conditions. Many men report avoiding activities such as swimming, wearing fitted shirts, or engaging in intimate activities with partners because of their asymmetric appearance.
In our San Francisco and Marin County practice, Dr. Miguel Delgado frequently treats men with unilateral gynecomastia, including complex revision cases in which prior surgery elsewhere did not achieve satisfactory symmetry.
Key points to understand:
- Unilateral gynecomastia involves the enlargement of breast tissue in only one breast.
- It causes visible chest asymmetry, ranging from subtle to pronounced.
- The condition is typically benign but warrants medical evaluation.
- Psychological and social impacts are often significant.
- Effective surgical correction is available for persistent cases.
Unilateral vs. Bilateral Gynecomastia: Why One Side Only?
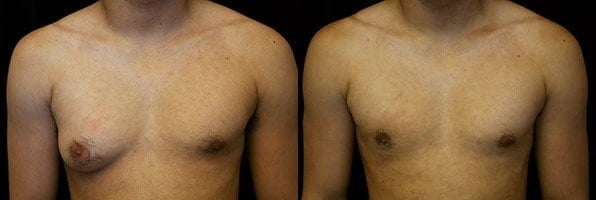
Gynecomastia in general develops when the balance between estrogen and testosterone in a male’s body tips in favor of estrogen, prompting glandular breast tissue to grow. This hormonal imbalance can occur at various life stages and from numerous causes.
The distinction between bilateral and unilateral forms comes down to symmetry. Bilateral gynecomastia affects both breasts, often to a similar degree, while unilateral gynecomastia presents with clear enlargement on only one side. In some cases, the “unaffected” side may have minimal involvement, but one side is distinctly more prominent.
One-sided gynecomastia can range from a subtle finding—palpable breast tissue only detectable upon examination directly under the areola—to a full, breast-like mound on one side of the chest that is visible through clothing. Clinical series have noted that the left side is often more commonly affected, though either side can develop gynecomastia.

Understanding the key differences:
| Bilateral Gynecomastia | Unilateral Gynecomastia | Asymmetric Gynecomastia (refers to both sides being affected but to noticeably different degrees) |
| Both breasts are enlarged, often symmetrically | One breast is clearly larger, creating asymmetry | Both sides are involved, but with a significant difference in size |
| Less visually obvious asymmetry | Asymmetry is often more visually obvious and emotionally distressing | One side is distinctly more prominent than the other |
| Either side can be affected | Left-sided involvement is reported more frequently in clinical literature | Either subtle or dramatic presentations are possible. |
How Common Is One-Sided Gynecomastia?
Gynecomastia is surprisingly prevalent across the male lifespan. It occurs in over half of male newborns due to maternal estrogen levels, affects up to 60–70% of pubertal boys as a temporary condition, and increases again in men over 50 due to age-related changes in hormone levels. Within this broader population, a meaningful subset presents with unilateral or clearly asymmetric gynecomastia.
Research indicates that although bilateral involvement is more common, approximately 10–35% of cases of gynecomastia involve unilateral or predominantly unilateral enlargement. It’s worth noting that mild asymmetry between the two sides of the chest is normal in many men. True unilateral gynecomastia, however, involves palpable glandular tissue concentrated on one side, creating a noticeable difference.
Prevalence insights:
- Gynecomastia affects the majority of males at some point in life.
- Pubertal gynecomastia (adolescent gynecomastia) is especially common, affecting over half of teenage boys.
- Roughly 10–35% of all cases of gynecomastia present unilaterally.
- About 25% of cases of gynecomastia are classified as idiopathic gynecomastia (no identifiable cause). Idiopathic gynecomastia means there is no identifiable cause for the breast tissue enlargement.
- Even common conditions warrant evaluation to rule out rare but serious causes.
Causes and Risk Factors for One-Sided Gynecomastia
Hormonal Causes Affecting Breast Tissue
The most frequent driver of gynecomastia is a shift in the estrogen-to-androgen ratio. During puberty, temporary fluctuations in testosterone levels and estrogen levels commonly cause pubertal gynecomastia, which typically resolves within one to two years. In older adult males, age-related testosterone decline combined with stable or increased estrogen can trigger breast tissue growth.
Conditions that raise estrogen levels or lower androgen levels also contribute. Obesity plays a significant role because fat tissue contains aromatase enzymes that convert androgens into estrogens. The pituitary and adrenal glands regulate hormone production, and dysfunction in these glands may contribute to hormonal imbalances.
Medication and Substance Causes
Up to 10–25% of gynecomastia cases are linked to medications or substances. Common culprits include:
- Anabolic steroids and prohormones used for bodybuilding
- Anti-androgen medications such as finasteride and spironolactone
- Medications used to treat prostate cancer
- Certain anti-anxiety medications and antipsychotics
- Some heart medications and anti-ulcer drugs
- Illicit drugs, including marijuana and opioids, that alter hormones
- Chronic alcohol use
Systemic Disease Risk Factors
Several health conditions can disrupt hormone metabolism and contribute to gynecomastia:
- Liver disease or liver failure (impairs estrogen breakdown)
- Kidney failure (affects hormone clearance)
- Thyroid disease, particularly hyperthyroidism
- Klinefelter syndrome (a genetic condition with an extra X chromosome)
- Testicular tumors or testicular tumours presenting with hormone production
- Adrenal tumors secreting estrogen or human chorionic gonadotropin
Local and Rare Causes
Sometimes the cause is localized rather than systemic:
- Prior trauma or hematoma that remodels into fibrous tissue
- Benign masses such as lipomas or cysts
- Male breast cancer (rare but critical to exclude, especially with a hard, fixed, unilateral breast mass)
- Genetic predisposition affecting one side’s tissue sensitivity
Pseudogynecomastia—the accumulation of adipose tissue rather than true glandular tissue—can also create an asymmetric chest appearance, sometimes masking or exaggerating underlying gynecomastia. Pseudogynecomastia refers to chest enlargement caused by fat accumulation rather than glandular tissue.
Breast Asymmetry: Understanding the Difference
Breast asymmetry is a common finding in both men and women, referring to a noticeable difference in size, shape, or contour between the two sides of the chest. In many cases, mild asymmetry is completely normal and may go unnoticed. However, when the difference is caused by the development of excess glandular tissue in only one breast, it is classified as unilateral gynecomastia.
Unlike general asymmetry, which might simply reflect natural variations in muscle or fat distribution, unilateral gynecomastia involves a true increase in glandular tissue on one side. This means that only one breast becomes enlarged, often resulting in a more pronounced and visible chest imbalance. For many men and adolescent boys, having only one breast affected can be especially distressing, as the asymmetry is more obvious and can impact self-confidence, clothing choices, and participation in activities.
Understanding whether your breast asymmetry is due to benign variation or excess glandular tissue is essential for determining the right course of action. If you notice a firm or rubbery mass beneath the nipple of only one breast, or if the difference in size is significant and persistent, it’s important to seek evaluation from a board-certified plastic surgeon. Proper diagnosis ensures that any underlying causes are addressed and that you receive the most effective gynecomastia treatment to restore a balanced, masculine chest contour.
Symptoms and When to Be Concerned
Most men with unilateral gynecomastia first notice something feels different on one side of the chest. You might feel a lump or growth directly beneath the nipple, notice visible asymmetry in T-shirts, or observe that one nipple appears puffier than the other.
Common Benign Symptoms
The typical presentation includes:
- A rubbery or firm glandular tissue disk directly beneath the areola on one side
- Visible breast mound or puffy nipple creating asymmetry
- Mild tenderness or soreness, especially during early growth
- Stretching or itching of the overlying skin as the tissue expands
- Sensitive nipples on the affected side
Warning Signs of Male Breast Cancer Requiring Prompt Evaluation
Certain features raise concern for more serious conditions, including male breast cancer or other male breast disease, and warrant immediate medical attention:
- A very hard, irregular, or fixed mass not centered under the nipple
- Nipple retraction, scaling, crusting, or bloody nipple discharge
- Rapid growth over just a few weeks
- Enlarged lymph nodes or firmness in the armpit area
- History of breast carcinoma in the family
- Prior chest radiation or known risk factors for breast cancer
While most cases in adolescent males and young men are benign, any new unilateral breast mass should be evaluated by a board-certified plastic surgeon or physician experienced in male breast conditions.
Diagnosis: How We Evaluate One-Sided Gynecomastia
Unilateral gynecomastia is ultimately a diagnosis of exclusion. Before confirming benign gynecomastia, other causes—including malignancy—must be systematically ruled out.
Clinical Evaluation
The evaluation begins with a thorough history and clinical examination:
- Detailed history covering age at onset, speed of growth, duration of symptoms
- Complete medication review, including supplements, steroids, and over-the-counter products
- Questions about alcohol, marijuana, and other substance use
- Assessment of symptoms suggesting systemic illness
- Physical exam of both breasts, the chest area, abdomen, and testes
- Evaluation for clinical features of endocrine disorders
During a routine physical examination, the physician will palpate for palpable breast tissue directly beneath the areola, distinguishing firm glandular tissue from softer adipose tissue. The location, consistency, and mobility of any mass help differentiate gynecomastia from other conditions.
Diagnostic Tests
When indicated, additional testing may include:
- Blood work to check hormone levels (testosterone, estradiol, luteinizing hormone, FSH, prolactin)
- Human chorionic gonadotropin levels to screen for certain tumors
- Liver and kidney function tests
- Thyroid function evaluation
- Breast ultrasound (most common initial imaging)
- Mammography or MRI in older men or atypical presentations
- Testicular ultrasound if a testicular mass or tumors are suspected
In adolescents with classic pubertal gynecomastia and no concerning features, extensive testing may not be necessary. However, documentation and appropriate follow-up remain important.
At Dr. Delgado’s practice, diagnostic steps are tailored to each patient’s age, history, and physical findings—prioritizing safety while avoiding unnecessary testing.
Non-Surgical Management and Observation
Treatment for unilateral gynecomastia depends on the patient’s age, the underlying cause, how long the condition has been present, and the degree of emotional distress it causes. For some patients, particularly younger individuals with recent-onset gynecomastia, observation may be appropriate.
Watchful Waiting Strategies
For prepubertal gynecomastia and pubertal cases:
- Typical observation period of 12–24 months to allow natural resolution
- Regular re-examinations to monitor for regression, stability, or progression
- Clear criteria for transitioning to active treatment if tissue persists beyond 1–2 years
- Consideration of intervention sooner if pain or a significant psychosocial impact occurs
Studies indicate that up to 90% of cases of pubertal gynecomastia resolve spontaneously within 2 years.
Lifestyle and Medical Measures
Several approaches may help address reversible causes:
- Discontinuing or changing causative medications under medical supervision
- Avoiding anabolic steroids, prohormones, and hormone-altering substances
- Weight loss through a healthy diet and regular exercise to reduce excess fat
- Referral to endocrinology for hormone-modulating medications in select early cases
- Aromatase inhibitors or selective estrogen receptor modulators (like tamoxifen) may be considered. Aromatase inhibitors are medications that block the conversion of androgens to estrogens, while selective estrogen receptor modulators (like tamoxifen) block estrogen effects in breast tissue.
It’s important to understand that while exercise can improve overall chest contour by reducing fat, true breast glandular tissue does not shrink significantly with exercise alone. Once fibrosis develops—typically after about 12 months—the tissue becomes essentially permanent.
The bottom line: Non-surgical options have their place, but for long-standing unilateral gynecomastia, surgery is usually the most reliable path to restore symmetry.
Surgical Correction: How One-Sided Gynecomastia Is Treated
Surgery is the definitive gynecomastia treatment for persistent unilateral gynecomastia that has not improved with time or medical management. Surgical removal of excess tissue is often necessary when conservative measures fail or when malignancy cannot be excluded. Unilateral gynecomastia surgery offers predictable results and high satisfaction rates when performed by an experienced surgeon. As highlighted in breast cancer res treat literature, a comprehensive approach to breast disease management—including early diagnosis and tailored interventions—is essential for optimal outcomes in both benign and malignant breast conditions.
Surgical Goals
The objectives of male breast reduction for one-sided gynecomastia include:
- Remove excess glandular tissue and, if present, excess fat from the enlarged breast;
- Create a flat, masculine chest contour matching the opposite side;
- Subtly adjust the “normal” side if needed, so both sides appear naturally similar;
- Minimize visible scarring; and
- Reduce the likelihood of recurrence.
Techniques Used by Dr. Delgado
Dr. Delgado employs several techniques tailored to each patient’s anatomy:
- Direct Excision: Removal of firm glandular tissue through a small incision along the areola border
- Liposuction: Contouring of surrounding fat to feather the chest into adjacent areas
- Combination Approach: Most cases benefit from both excision and liposuction for optimal results
- Tissue Removal: Careful extraction of excess tissue while preserving natural contours
- Areola Adjustment: Attention to areola size, position, and nipple projection for symmetry
Anesthesia and Setting
The procedure is typically performed under general anesthesia in Dr. Delgado’s fully accredited surgical facility, Marin Cosmetic Surgery Center, with an emphasis on patient safety and privacy. Duration ranges from approximately 1–2 hours, depending on complexity and whether both sides require adjustment for optimal symmetry.
Each case is individualized. Some men have primarily glandular tissue, others mainly fat, and some require revision surgery to correct unsatisfactory results from previous procedures.

Dr. Delgado’s Approach
Dr. Delgado focuses on achieving:
- Natural-looking, athletic results
- Minimal visible scarring
- Reduced likelihood of recurrence
- Balanced, symmetric appearance between both sides
Recovery, Scars, and Long-Term Results
Recovery from unilateral gynecomastia surgery is typically straightforward, though adherence to post-operative instructions is essential for optimal outcomes.
Recovery Timeline
What to expect after male breast reduction surgeries:
- Return home the same day of surgery.
- Resume desk work and light activities within a few days.
- Light exercise is permitted after approximately 1–2 weeks.
- Avoid heavy lifting and chest workouts for 4–6 weeks.
- Wear compression garments as directed (typically 4–6 weeks).
Early Side Effects
During the initial healing phase, you may experience:
- Swelling and bruising on the operated side
- Mild to moderate tightness or soreness
- Temporary numbness or altered nipple sensation (usually improves over several months)
- Mild drainage at incision sites
Scar Appearance
Surgical excision scars are typically:
- Located along the border of the areola (well-concealed)
- Small liposuction access points are minimal and fade significantly
- Initially pink or red, fading over several months
- Best managed with sun protection and silicone-based scar products
Long-Term Outcomes
The majority of patients experience excellent results:
- A flatter, more symmetrical chest is revealed once swelling subsides (typically 3–6 months).
- Recurrence is uncommon when underlying causes (steroids, certain medications) are addressed.
- Significant emotional benefits are achieved; patients report confidently wearing fitted shirts, swimming without a shirt, and improved intimacy.
- Resolution of emotional distress that prompted surgery occurs.
Dr. Delgado closely monitors patients throughout recovery and adjusts recommendations based on their specific procedure and lifestyle needs.
Cost Considerations and Insurance Questions
The cost of unilateral gynecomastia surgery varies based on several factors, including the complexity of the case, operating time, anesthesia requirements, and whether both sides need adjustment to achieve optimal symmetry.
Typical Cost Components
Fees generally include:
- Surgeon’s professional fee
- Anesthesia fee
- Facility fee for use of an accredited operating room
- Preoperative testing, if required
- Postoperative compression garments and follow-up care
Insurance Coverage
Most insurance companies classify gynecomastia surgery—including correction of unilateral cases—as a cosmetic procedure and do not provide coverage. However, policies vary, and coverage may occasionally be available when a documented medical necessity is present.
Our recommendation: Contact our office directly for a personalized fee estimate following your consultation. We can discuss available payment options and financing arrangements to help make treatment accessible.
Why Choose Dr. Miguel Delgado, M.D. for One-Sided Gynecomastia Correction?

Correcting unilateral gynecomastia requires a surgeon who understands both the technical aspects of achieving symmetry and the emotional impact of this condition on patients. Dr. Miguel Delgado, M.D., is a board-certified plastic surgeon with extensive experience in gynecomastia surgery, including challenging unilateral and revision cases.
Credentials and Experience
- Decades of specialized experience in male chest contouring;
- Practice locations in San Francisco and Marin County;
- Fully accredited in-office surgical facility prioritizing safety and privacy;
- Extensive portfolio of gynecomastia before-and-after results, including asymmetric cases; and
- Recognized expertise in treating gynecomastia of all types and complexities.
Our Approach
What sets Dr. Delgado’s practice apart:
- Thorough consultation distinguishing true gland from fat and ruling out other pathologies;
- Honest discussion of all treatment options—observation, medical management, or surgical correction;
- Customized surgical planning that balances the treated side with the opposite chest;
- Focus on achieving a natural, masculine chest contour without an “operated” appearance; and
- Attention to excess skin management when needed for optimal results.
Patient-Focused Care
From your first consultation through final follow-up:
- Clear pre-operative education and realistic expectations
- Compassionate, judgment-free environment
- Close monitoring throughout the healing process
- Commitment to long-term results and patient satisfaction
- Availability for revision surgery when patients come from other practices
Next Steps: Consultation and How to Get Help

If you or your son has noticed one-sided breast enlargement, the most important step is seeking professional evaluation rather than ignoring the issue or hoping it will resolve on its own. While many cases—particularly in adolescent males—improve over time, persistent or distressing cases benefit from expert assessment.
How to Schedule
Getting started is straightforward:
- Free virtual consultations are available for convenience.
- In-office consultations are available at our San Francisco and Marin County locations.
- Patients from across Northern California and beyond are welcome.
- Efficient scheduling minimizes wait times.
What to Expect at Your First Visit
Your consultation will include:
- A private, judgment-free discussion of your concerns;
- Review of your medical history, medications, and goals;
- Physical examination to assess the nature and extent of the condition;
- Preliminary treatment recommendations (observation, further testing, or surgical excision); and
- Clear answers to your questions about surgery, recovery, and cost.
Please bring: Prior test results, a complete medication list, and any questions you may have about the process.
Unilateral gynecomastia can be effectively corrected, helping you develop gynecomastia-free confidence and return to activities you’ve been avoiding. Whether you’re dealing with recent changes or have lived with chest asymmetry for years, seeking expert evaluation is often the most important first step toward reclaiming your comfort and self-assurance.
Schedule your free consultation today and take the first step toward a more balanced, confident you.
FAQs About Unilateral Gynecomastia
What causes one-sided gynecomastia?
One-sided gynecomastia, or unilateral gynecomastia, arises when excess glandular breast tissue develops in only one male breast, resulting in asymmetry. The underlying causes are often similar to those of bilateral gynecomastia but can manifest unevenly due to various factors.
The primary cause is hormonal imbalance, specifically an increased estrogen-to-testosterone ratio. Estrogen promotes breast tissue growth, while testosterone inhibits it. When this delicate balance shifts—due to puberty, aging, medications, or health conditions—breast tissue can enlarge. In unilateral cases, this imbalance may affect one side more prominently because of localized differences in tissue sensitivity or hormone receptor density.
How do you fix unilateral gynecomastia?
Correcting unilateral gynecomastia involves a tailored approach depending on the severity, duration, and underlying cause of the condition. Treatment options range from watchful waiting and medical management to surgical intervention. Here’s a detailed overview of how unilateral gynecomastia can be effectively addressed:
1. Observation and Lifestyle Adjustments
For many adolescent males and some adults, unilateral gynecomastia may resolve on its own over time, especially if it is related to pubertal hormonal changes. During this period, maintaining a healthy diet and regular exercise can support overall hormonal balance and reduce excess adipose tissue that may contribute to chest asymmetry. Avoidance of substances known to cause hormonal disruption—such as anabolic steroids, certain medications, alcohol, and illicit drugs—is also recommended.
2. Medical Treatment
When hormonal imbalances are identified as the underlying cause, medical therapies may be considered. Medications such as selective estrogen receptor modulators (SERMs), including tamoxifen, and aromatase inhibitors can reduce breast glandular tissue by blocking estrogen effects or decreasing estrogen production. These treatments tend to be most effective when started early in the course of gynecomastia development. However, they may have side effects and are not suitable for all patients.
3. Surgical Correction
Surgery remains the most reliable and definitive treatment for persistent unilateral gynecomastia, particularly when the breast enlargement has been present for more than 12 months or causes significant emotional distress. The goal of unilateral gynecomastia surgery is to remove excess glandular tissue and fat to restore a balanced and masculine chest contour.
Dr. Miguel Delgado, M.D., utilizes a combination of techniques tailored to each patient’s anatomy:
- Direct excision of firm glandular tissue through a discreet incision, typically along the areola border.
- Liposuction to remove excess fat and sculpt the chest for a natural appearance.
- Skin tightening and areola reshaping are necessary to address excess skin or nipple asymmetry.
The surgery is performed under general anesthesia in a fully accredited surgical facility, ensuring patient safety and comfort. Recovery typically involves wearing compression garments, managing swelling and bruising, and adhering to postoperative care instructions to optimize outcomes.
